Global Science for Health Worldwide
Tropische ziekten, hiv/aids, tuberculose en ontoereikende gezondheidszorg beïnvloeden de levens van miljarden mensen wereldwijd.
Het Instituut voor Tropische Geneeskunde (ITG) in Antwerpen (België) zet zich sinds 1906 in voor de vooruitgang van wetenschap en gezondheid voor iedereen, via innovatief onderzoek, geavanceerd onderwijs, professionele medische dienstverlening en capaciteitsuitwisseling met partnerinstellingen in Afrika, Azië en Latijns-Amerika. Ons doel is de wereldwijde impact van ziekten en gezondheidsproblemen op bevolkingsgroepen te verminderen.
Wetenschappelijke excellentie en maatschappelijke relevantie zijn voor ons twee kanten van dezelfde medaille.

Het ITG viert 120 jaar wetenschap
Al meer dan een eeuw zet het Instituut voor Tropische Geneeskunde (ITG) zich in voor betere gezondheid en wetenschap in de wereld, via baanbrekend onderzoek, toonaangevend onderwijs en wereldwijde zorgverlening. Tijdens ons jubileumjaar blikken we terug op waar het begon en richten we ons op een toekomst die gevormd zal worden door onze grensverleggende doorbraken.
In de kijker

Dien je abstract in voor het ITG-Colloquium 2026
De 66e editie van het ITG-Colloquium 'Health in Motion: Infectious Diseases on the Move' vindt plaats in Addis Abeba, Ethiopië, van 15 tot 17 november 2026. Dien je abstract in!
Deadline: 19 mei 2026

Het ITG blaast 120 kaarsjes uit
2026 wordt een bijzonder jaar, want het ITG bestaat 120 jaar. Het hele jaar zal gevuld zijn met boeiende verhalen en inspirerende evenementen.

Win jij de Nature Inspiring Women in Science Awards?
De prestigieuze Inspiring Women in Science Awards bieden je de kans om je prestaties onder de aandacht te brengen of de bijdragen van een collega te steunen. Het programma kent een prijs van $ 50.000 toe.
Deadline 2026: 8 april 2026

Podcast seizoen 3 nu uit!
Luister naar The Road to Zero, het derde seizoen van onze bekroonde podcast Transmission, op je favoriete podcastplatform!🎧

Onze kliniek
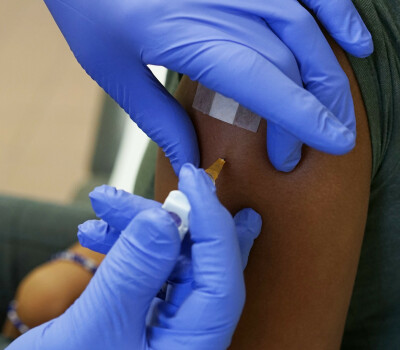
Onze polikliniek is gespecialiseerd in de diagnose, behandeling en zorg van hiv/aids en andere seksueel overdraagbare infecties, reisgeneeskunde, tropische geneeskunde en infectieziekten.
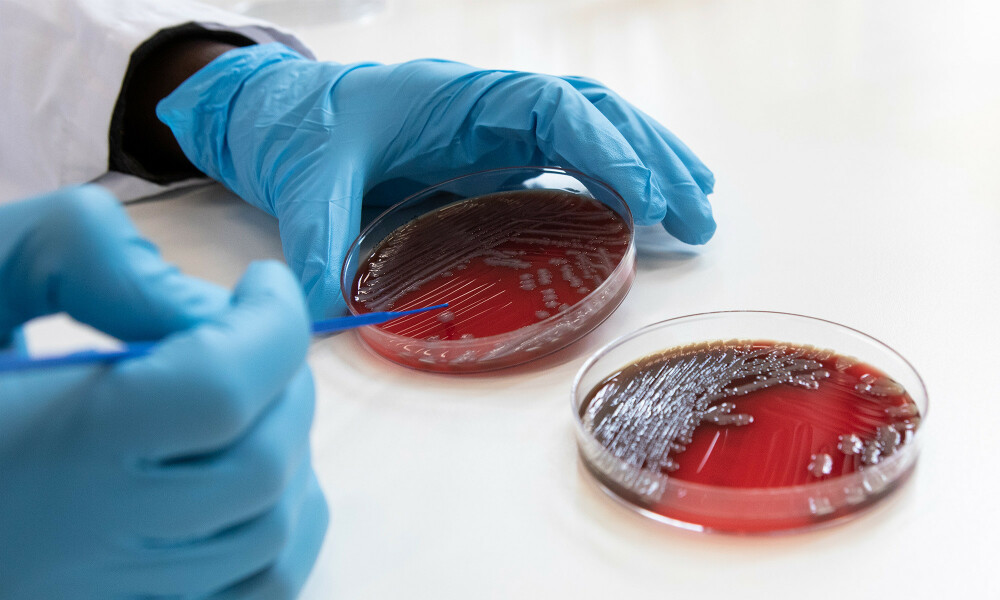
Ons onderzoek
We vergroten de kennis over tropische ziekten en infectieziekten en pakken belangrijke gezondheidsuitdagingen aan, met speciale aandacht voor omgevingen met weinig middelen en kwetsbare bevolkingsgroepen.
Onze opleidingen
We bieden masterprogramma's, postgraduate certificate-programma's en korte cursussen aan op het gebied van tropische geneeskunde, internationale volksgezondheid en Global One Health voor professionals van over de hele wereld.

Onze partners
We werken samen met talloze partners verspreid over drie continenten op het gebied van institutionele capaciteitsuitwisseling en samenwerking.

Maak een afspraak
Consultaties in onze polikliniek zijn uitsluitend op afspraak. Boek je afspraak ruim op tijd, want in de lente en de zomer kan de wachttijd lang oplopen.

Contact
Voor medisch advies moet je een afspraak maken in onze kliniek, maar voor andere zaken kan je gemakkelijk contact met ons opnemen.
Webshop
Neem een kijkje in onze webshop en koop je ITG-hoodie, notitieboekje, sokken, boc 'n roll en nog veel meer!
Evenementen
Bekijk alle evenementenIDAHOT - hiv-zorg en stigma
Aula Janssens, Campus Rochus, Sint-Rochusstraat 43, 2000 Antwerpen
PhD defence Diana Sagastume
ITG Onderwijscampus Rochus, Aula P.G. Janssens, Sint-Rochusstraat 43, 2000 Antwerpen